
Read and buy our books online

The MacLeod Laboratory offers a complete Infertility evaluation, treatment for Primary or Secondary Infertility
Read Online Buy it on amazonContact us Confidentially
A. Toth, M.D.
Obstetrician, Gynecologist, & Pathologist
email drtoth@fertilitysolution.com
Treatment for Chronic Prostatitis
- Historical Perspective
- Clinical Course and Symptoms of Acute and Chronic Prostatitis
- Evaluation of Patients with Prostatitis
- Treatment for Acute and Chronic Prostatitis, Seminal Vesiculaitis, Epididymitis and Orchitis with Direct Injection Therapy
- Late Sequels of Chronic Prostatitis
- Seminal Vesiculitis
- Epidydimitis and Orchitis
- Technical Details of Injection Therapy
- Illustrations for the Transrectal Injection Technique
Historical perspectives
Eight years ago The MacLeod Laboratory started offering direct intra-prostatic injections for the treatment of chronic prostatitis.A retrospective analysis of the data showing the changes in pre and post therapy symptom scores of individual patients is under way. The initial analysis shows very favorable results. I would like to explain the logic behind the procedure and how I took it upon myself as a gynecologist and pathologist to venture into the field of urology and offer an alternative approach to treat one of men’s most troubling and yet most neglected diseases, prostatitis.
During the last five years approximately four hundred males with prostatitis have been treated at The MacLeod Laboratory. A study of these patients and their response to treatment has increased our understanding of the disease itself and the devastating effect chronic prostatitis has on all aspects of a man's life.
Chronic prostatitis can gradually decrease a man’s physical performance and eventually exhaust his mental reserves. His social and sexual life suffer. Bacterial prostatitis can alter or completely impair his partners fertility. Bacteria harbored in the inflamed prostate are transferred into the female's uterus and can cause functional and structural damage to her reproductive tract and interfere with the course of a normal pregnancy. These same bacteria can leave behind life-long stigmata on the newborn.
Even while childbearing is not desired bacteria transferred from an infected prostate can change female pelvic function. The infection alters a woman's hormonal balance, affecting libido and causing other sexual dysfunctions.
As a gynecologist and pathologist I have witnessed the effect of this disease on my female patients who have suffered, sometimes irreversibly from bacteria transmitted by their infected partners. It is clear therefore that my approach to treating prostatitis is drastically different from the isolationist approach of my urologist colleagues. My background as a pathologist first and then a gynecologist– a rare combination in medicine- gives me a unique vantage point. My first fifteen years, after completing medical school, were spent in the laboratory with a microscope, giving me a three dimensional view of diseases and a keen interest in searching for cause and effect correlations in all diseases.
The following thirty years I spent as a practicing clinician in gynecology and obstetrics. My practice was almost exclusively limited to treating infertility and genital tract infections. During these years I became convinced that there are two incomplete branches of medicine, gynecology and urology which should not be studied separately and cannot be understood separately. Males and females are medically interconnected by the fact that sexual intercourse allows not only for reproduction but facilitates the of bacterial flora between the partners.
Due to the profound effect of prostatitis causing bacteria on reproduction in both males and females, they have to be mentioned in the context of reproduction. If you are a young male and you are yet to father a child, prostatitis could affect your fertility and the health of your future children. If you are an older man who was never able to have children, prostatitis could have contributed to your infertility.
Being an infertility specialist and treating men and women for infertility, I have worked closely with urologists. As a pathologist with extensive training in microbiology, it did not take long for me to realize that the overwhelming majority of all infertility cases are infection related. More importantly, the understanding that these infections are shared by both sexes became the paradigm of my medical practice.
While the prostate serves as a sphincter for both the urine and seminal fluid, its more important function is to trap microbes through an elaborate immunological mechanism. The prostate, in response to bacterial invasion produces a host of antibodies. Some of these antibodies are less specific than others and the sperm themselves may get into the crossfire causing anti-sperm antibodies.
This was basically when I began treating the prostate, of asymptomatic infertile males, but later as word traveled — single and married men started to consult me for the sole purpose of receiving therapy for symptomatic prostatitis.
The majority of my patients come to me with the diagnosis of nonbacterial prostatitis. In our laboratory it is exceedingly rare to find negative EPS (expressed prostatic secretion) or semen cultures. Due to lack of final proof we always used the term "association" of a bacterium with certain conditions rather than labeling them as being the cause of that condition. The prescribed antibiotic therapy and the subsequent favorable clinical and reproductive outcome seemed to confirm that we are on the right track. Initially, we treated our patients with usually recommended oral therapy. Our frustration with returning symptoms and positive bacteria findings after repeated oral therapies prompted us to use multi-drug regimens and later intravenously administered antibiotics. Recalling the microscopic image of an enlarged prostate with extensive scarring shielding pockets of bacteria and inflammatory cells, it was easy to understand that oral or even intravenously given antibiotics cannot reach proper concentration in those areas. The introduction of directly injecting antibiotics into the prostate gland delivering 1000 to 2000 fold the concentration of antibiotics than any other previously practiced approach became a logical sequel to our therapy. The injection therapy is rewarded with much improved symptomatic response and great reduction in positive post therapy semen cultures.
Clinical Course and Symptoms of Acute and Chronic Bacterial Prostatitis
Acute and chronic prostatitis is a continuum of the same disease. The initial symptoms are modified by a series of factors, most importantly the activation of the immune system and the antibiotics received for the initial episode. The interaction of these factors with the pathogenic bacteria will determine when the acute phase becomes chronic and when during the chronic infection an acute flair up occurs.Entry of bacteria into the male genital canal takes place through the urethra and the great majority of cases follow a sexual intercourse.
The first symptoms of acute prostatitis are urethral burning or pain at the tip of the penis and as the bacteria multiply and progress along the urethra, some patients can sense the extent of progression. At this stage the patient can report clear, watery, yellowish or even bloody discharge. Next the infection progress to the prostatic urethra and promptly spreads to the bladder and into the prostate itself. Symptoms in this phase of the infection affect the urinary tract with painful urination, difficulty starting urination, bladder spasm, a feeling of incomplete emptying following urination, or frequent urination at night (nocturia). Often, involvement of the posterior urethra will affect the ejaculatory ducts causing painful ejaculation or difficulty with ejaculation including premature ejaculation and difficulty maintaining an erection. It is rare to encounter patients who have reached this stage of the disease and have not already sought therapy. More about acute prostatitis, click above.
Without antibiotic therapy
The infection will advance to the epididymis and testicles and painful swelling of those organs is usually followed by tissue destruction and occlusion of the sperm carrying ducts.
Virulent bacteria can cause rapid disease progression. Within days, generalized symptoms will develop, sometimes to a state of sepsis.
The immune system is primed during the first infection and antibody production begins. Several factors will determine the long-term course of the infection. Among them the most important are the virulence of the infecting bacteria and the state of the immune system. Ultimately the disease will follow an erratic course with gradual scarring and obstruction of the vital duct system and enlargement of the prostate. Once the sperm forming elements of the testes are destroyed, the volume of the testes diminishes and their consistency softens. The obstructed ducts in the epididymis can form small cystic nodules, called spermatocele. Complete obstruction of the duct system will lead to sperm free ejaculate - azoospermia.
With antibiotic therapy
Most patients with acute infection visit a urologist or the local family physician. The majority will have a urine analysis and inevitably leave the office with a prescription for a ten-day or two week course of antibiotic. Often by the end of this short course of antibiotic therapy, most if not all the urethritis and bladder symptoms disappear and the patient feels well. With a functioning immune system and antibiotic therapy the progression of the condition may abort at any level, or if the antibiotic therapy was inadequate it can progress into the second phase with persisting symptoms fluctuating with various intensity (typical for Chlamydial infections).The second phase of the infection that follows is caused by persistent bacteria in the prostate, and the related symptoms are numerous: urinary frequency, urinary urgency, pain in the pelvic area aggravated by long term sitting, pain or discomfort during or after ejaculation, discomfort with aching pain radiating from the rectum, feeling of golf ball size mass in the pelvis or rectum, discomfort/pain in penis, supra pubic pain, pain between scrotum and anus radiating to tailbone, lower back pain, groin pain, pain during urination (disuria), frequent urination at night (nocturia), reduced stream, incomplete emptying of the bladder, hesitancy, discomfort or relief after bowel movement, clear discharge from the penis during difficult bowel movements. Secondary to the persisting symptoms, anxiety, depression, loss of self-esteem, loss of sex drive and social withdrawal can develop.
The nature of prostatitis is a recurring disease that is treated with repeated oral antibiotic courses. A high number of patients will undergo cystoscopy at the beginning of this process, a procedure that hardly ever alters the management and in my opinion is not justified.
The findings of a physical examination will change as the disease progresses. A digital rectal exam in the early phase will reveal a soft, boggy and very tender prostate and the patient will signal marked discomfort when EPS (Expressed Prostatic Secretion) is collected. Chronic infection with the formation of scar tissue will form firm nodules within the prostate, which are readily detected with manual examination. As scarring progresses the yield of EPS diminishes. Positive bacteria cultures from the EPS in bacterial prostatitis are highest in the early phase of the acute infection, with white and red blood cells and bacteria present. In the chronic phase the white blood cells will gradually diminish and the chance for bacteria isolation diminishes. Erroneously, this phase of the infection is commonly referred to as nonbacterial prostatitis.
During my ten years as a practicing pathologist I have seen numerous surgical specimens removed either for benign prostate hypertrophy or for prostate cancer. All of these specimens, without exception, revealed signs of infection. It is therefore not an unreasonable hypothesis that chronic prostatitis, prostate hypertrophy and prostate cancer represent a continuum of a disease process, and effective eradication of the infectious element should be pursued aggressively.
The Evaluation of Patient with Prostatitis
Functional considerations: The prostate gland serves three basic functions:
1. As a stopgap, it determines whether the man is urinating or ejaculating
2. As an immunological organ, it secretes bactericidal fluid that mixes with the ejaculate and protects spermatozoa
3. Not unlike the tonsils, it serves as a filter for bacteria entering the male body through the urethra. The prostate entraps and sequesters invading bacteria, and undergoes inflammatory and structural changes. In a stationery organ this process would ideally serve the body. As the prostate gland contracts every time a man ejaculates or urinates, these sequestrations are imperfect. Escaping bacteria are squeezed into other healthy parts of the prostate. If they enter the ejaculate, the bacteria will enter the female partner’s reproductive canal and may damage both the physical integrity and reproductive performance of the female genital tract. Once pathogenic bacteria breach the prostate, ascending infection to the bladder and to the kidneys or descending infection to the epididymis can occur. I rarely see males with bladder infections or kidney infections in my practice. I meet patients with epididymal infections regularly.
The work up for prostatitis
The work up begins with the review of a detailed medical history and an objective evaluation of the patient’s symptoms. We adopted the NIH standard prostatitis questionnaire as seen here. A numerical score is given to the individual symptoms and they will be used later for comparison with the post therapy symptom index.Semen and urine analysis with culture studies are performed. Cultured organisms include: Chlamydia trachomatis (from the urethral swab), Mycoplasma group, complete screening for aerobic and anaerobic bacteria and yeast. Both urine and semen are examined for the parasite Trichomonas.
The next step is a physical examination of the external genitals. The prostate and seminal vesicles are evaluated first with digital rectal examination and then rectal sonography. Pictures taken during the sonographic examination are stored in the chart for documentation and for future reference.
An EPS (expressed prostatic secretion) sample is examined under the microscope for epithelial cells, bacteria and white and red blood cells. Similarly urine sediment is examined to rule out a cystitis component. If indicated the EPS is processed for different culture studies.
Two to three weeks are needed to complete the culture studies and antibiotic sensitivity.
Treatment of Acute and Chronic Prostatitis, Seminal Vesiculitis, Epididymitis and Orchitis
For acute prostatitis that is promptly treated with adequate antibiotics courses the cure rate is 100%. (See link above for acute prostatitis) The most effective therapy for prostatitis and seminal vesiculitis is direct transrectal injection of antibiotics. See Figure 1. below.When to inject the seminal vesicle?
It is probably a good habit to inject both seminal vesicles at least once even if there is no clinical or sonographic sign for involvement. Whether definite scarring of either the excretory duct or the gland itself is documented by sonography, every session of prostate injections should deliver part of the antibiotics into the seminal vesicles.Transperineal or Transrectal Injections?
We find the transperineal injection cumbersome. The discomfort for the patient is much less with transrectal injection. The transperineal injection needs local anesthesia of the deep tissues, therefore it takes longer and the aim of the 25G injection needle is compromised while traversing through several layers of the perineum.The main argument against the transrectal injections is the potential infection introduced through the puncture hole of the rectum. During the years we have performed a large number of injections through the rectum and have never experienced any infection-related complications. I attribute this to the broad-spectrum antibiotics we use and to the fact that the injected antibiotics, upon withdrawal of the needle, promptly fill the track of the needle, as witnessed on the sonogram screen.
Optionally prostatic massages can be performed to improve blood circulation and antibiotic distribution. For more information about prostatic massages click here.
It is our belief that a large percentage of the cases of prostatitis are either caused by or aggravated by Chlamydia infection. The therapeutic considerations should follow the natural course of this bacterium’s life cycle. As the patient receives repeated courses of antibiotics the growth rate of Chlamydia will greatly diminish and eventually intracellular, spore forms will develop. The inactive phase of Chlamydia does not respond to therapy. Adding steroids to the injected cocktail will accelerate intracellular replication of resting Chlamydia forms and, following cell destruction, will bring the elementary bodies into the extracellular space for antibiotics to gain access to them.
Due to unpredictable availability of residual Chlamydia for therapy there is always a great uncertainty in judging the success of the first course of therapy.
Follow up booster injections, two or three per session, are recommended, three, six and nine months following the initial therapy.
Late sequels of chronic prostatitis
The symptoms fall into three categories.1. Localized symptoms in the pelvic area due to inflammation, physical enlargement, and compression of surrounding tissue caused by the prostate itself. Among these are the bladder-related symptoms; nocturia, difficulty voiding/disuria, incomplete bladder emptying, change in urine stream, and post-voiding dribbling of the urine. Involvement of the ejaculatory duct and the seminal vesicle out flow duct can result in premature ejaculation or diminished ejaculatory volume. Irritation of the surrounding nerves and muscles, the formation of peri prostatic adhesions, scarring around the seminal vesicles will cause pain localized behind the pubic bone or lower back or bilaterally if the seminal vesicles are also involved. If the ductus deferens is involved, especially if the infection progresses to the epididymis, testicular pain can develop.
2. Immune response secondary to the inflammation (especially in cases of Chlamydia related prostatitis). A variety of these symptoms can occur including Reiter’s syndrome. In addition, any joint, synovium can be affected and I have seen several cases where a recurrence of the infection resulted in a tingling sensation in different parts of the body. In our practice, antibiotic therapy has reversed several cases of severe arthritis that developed after the onset of a Chlamydia infection. Immune suppression therapy had been unsuccessful in alleviating the arthritic symptoms but the antibiotic therapy provided a permanent cure.
3. Personality changes and sexual disorders associated with prostatitis. Studies have shown that patients with chronic prostatitis often fear of developing prostate cancer, fear of having a sexually transmitted disease, erectile dysfunction and marital problems. A significant number of patients report decreased libido and often exhibit nervous behavioral patterns. I have had patients who reported thoughts of suicides.
Do vertically transmitted infections cause prostatitis?
When a 17-year-old virginal male presented with a series of symptoms typical for chronic prostatitis, I suspected for the first time that vertically transmitted infections could lead to prostatitis. Analyzing the parent’s reproductive history, it became apparent that a variety of infectious complications were obvious in both the father’s and mother’s genital tracts during their reproductive years and that the couple suffered from infertility, miscarriages, and even while the mother was pregnant with my patient, the pregnancy was complicated by an infection. I entertained the possibility that the same infection that compromised the parents’ reproductive performance was the cause of my patient’s chronic ear infections, chronic tonsillitis, and upper respiratory tract infections during his early life. My assumption was that the intrauterine and intravaginal bacterial flora during his intrauterine life gained access to his prostate during the pregnancy. The precise factors that allow these bacteria to multiply enough to cause a symptomatic infection remain a mystery. The case helped me to delineate a group of people whose infection is not a clear-cut sexually transmitted disease, but more likely a vertically acquired infection. Unfortunately, this group of patients will have a poorer response to therapy and will exhibit the above-mentioned psychological problems to an even greater degree. Following our therapy, the natural course of the disease will show an up and down course, not unlike a sinusoidal wave with diminishing amplitudes. Patients with strong psychological overtone of their disease will experience disproportionate symptom flare ups while on the upside slope of the first few post therapy sinus wave. This reaction can reach a state of total desperation. Before reaching for any physical remedy, such as pain medications, a new course of antibiotic, cystoscopy, prostate biopsy e.t.c. one should reassure the patient and explain the up and down course of the disease. A calm, reassuring and caring voice can do much more good then most of the other remedies combined.The major pitfalls in treating the first episode of prostatitis.
Seminal vesiculitis
Due to their anatomic proximity and a communicating duct system between the prostate and seminal vesicles, infections entering the prostate will find their way quickly into the seminal vesicles. Therefore, injection therapy for chronic prostatitis should always include treating the seminal vesicles at the same time.Within days, following the unset of urethritis, acute infection with a virulent strain of Chlamydia will spread along the surface mucosa of the urethra and most patients will recall the progression of this infection.
Once bacteria reach the posterior urethra, unchecked entry into the seminal vesicles and ductus deference will take place through the common ejaculatory ducts. Infection to the prostate proper will follow through the varying numbers of ducts the prostatic fluid is excreted into the posterior urethra.
On sonographic examination, tissue reaction to the progressing infection will show up very early. Clusters of scattered scarring outlining ductal structures appear in shapes of beads, or form grape like clusters within the prostate. A long lasting infection will cause scarring of the entire intraprostatic segments of both ductus deferentes and the terminal ducts of the seminal vesicles. An extreme case is the formation of the Double Gothic Arches. The two median segments of the arches represent the two ductus deferentes, while the lateral segments are the two excretory ducts of the seminal vesicles. Bilaterally, the tip of the arches represents the fusion of the two structures into the ejaculatory ducts.
Chronic infection within the seminal vesicles causes mild to significant scarring of the wall of the gland with diminished quantity of vesicular fluid visible. Sonographic examination will show clusters of ring like structures with or without fluid in the centers. Advanced cases can progress to complete obliteration of the entire gland with markedly diminished ejaculatory volume.
A subset of patients will present with acute fullness feeling in the deep pelvis shortly after the onset of urethritis and report diminished ejaculatory volume. Semen analysis may reveal high sperm count and reduced volume. The markedly dilated seminal vesicles, seen on the sonogram, help make the likely diagnosis of isolated, bilateral occlusion of the excretory ducts of the seminal vesicles.
In rare instances, seminal vesiculitis develops without any overt sign of prostatic infection. A vague feeling of discomfort, deep in the pelvis, unilateral or bilateral can be the only presenting symptom. If injection therapy is directed only to cure an assumed prostatitis, the results bound to be disappointing. While the symptoms may change marginally, the lower pelvic discomfort persists unless proper antibiotic cocktails are injected into the seminal vesicles. Since the seminal vesicles are much more sensitive to chemically irritating antibiotics then the prostate, significantly more analgesics should be offered prior to injecting concentrated solutions into the seminal vesicles.

1. Sonographic picture of a normal seminal vesicle: Note the tortuous, thin walled gland, evenly filled with secreted material.

2. Sonographic appearance of a seminal vesicle with acute obstruction of the excretory duct. Picture taken 15 minutes after ejaculation. The ejaculatory volume was 0.9 cc and the sperm count 512 million per ml.

3. Taken from a lateral angle. Sonographic image of Chlamydia infection forming beads like scarring along terminal ducts of seminal vesicle end ductus deference. Similarly, beads are outlining the prostatic urethra. Within the prostate, the infection forms clusters of small scars with or without calcification (Cluster of Grapes).
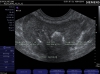
4. A chronic infection can cause scarring of the entire intraprostatic segments of both ductus deferentes and the terminal ducts of the seminal vesicles. An extreme case is the formation of the Double Gothic Arches. The two median segments of the arches represent the two ductus deferentes, while the lateral segments are the two excretory ducts of the seminal vesicles. Bilaterally, the tip of the arches represents the fusion of the two structures into the ejaculatory ducts.

5. A cluster of rings replacing the normal structure of a chronically infected seminal vesicle. The sonographic picture clearly shows the thickened walls with greatly diminished secreted material. The patient had an over twenty years long history of chronic prostatitis. The main symptom was low back pain.

6. Seminal vesicle shown in Figure 5 following antibiotic injection. Note dilated seminal vesicle with thickened wall, filled with the antibiotic solution.

7. Sonographic image showing a completely destroyed seminal vesicle, in a patient with end-stage seminal vesiculitis. Biopsy of seminal vesicle showed extensive scarring with numerous Chlamydia trachomatis elementary bodies.
Conditions related to seminal vesiculitis
A host of other ill defined pelvic conditions are either directly caused by or aggravated by inflammation of the seminal vesicles: pelvic floor dysfunction, myofascial trigger point dysfunction, pudendal nerve entrapment and so on. The recommended therapies are numerous: Prostatic Massage, Perineal or Pelvic Floor Massage, Myofascial Trigger Point Release, Pudendal Nerve Entrapment Therapy Biofeedback, Acupuncture and Psychological Support.In general, I have no objection to any of these therapies, provided proper antibiotic therapy is administered first.
Epididymitis and Orchitis
Functional Considerations and Pathogenesis of InfectionThe function of the epididymis is to collect the sperm formed in the testes through dozens of delicate tubules where the final maturation of the spermatozoa takes place. From there the ductus deferens carry the sperm through the prostate to the ejaculatory ducts. The epididymis is highly vascularized and the nourishing medium surrounding the tubules not only promotes sperm maturation, it is also a fertile ground for bacterial growth.
In epididymitis the infectious bacteria, most commonly Chlamydia trachomatis, arrives to the epididymis and a painful inflammation develops. The posterior aspect of the testis reveals the swollen and very tender epididymis. The entire organ or part of it can be affected. If the antibiotic therapy is inadequate, following repeated failed courses; the collective duct system is damaged and localized scarred nodules, called spermatoceles form. As the infection progresses, it will completely obstruct the duct system. Even after the symptomatic phase has subsided, the scarred areas become a source for bacteria, causing future flair ups or they can lead to asymptomatic bacteriospermia. In cases of orchitis, acute painful enlargement of the testis signals the bacterial invasion. This condition should be considered a reproductive emergency. Virulent bacteria rapidly destroy the sperm forming tubules and neglected cases can lead to severe oligospermia or azoospermia.
To avoid damaging the collecting duct system of the epididymis we only perform trans-cutaneous infiltration of the space around the epididymis.
Therapy
My choice of therapy for orchitis is intravenous antibiotics with broad coverage for Chlamydia trachomatis, aerobic and anaerobic bacteria. To avoid potential chemical damage to the delicate duct system by the concentrated antibiotics, I avoid injecting antibiotics directly into the testis.Technical Details of Injection Therapy
Advantages of Injection Therapy for Pelvic Infections in the MaleConcentration of antibiotics in the tissues can reach 1000 to 2000 folds that of the levels achieved through orally or even intravenously given antibiotics. No other organs are exposed to toxic levels of antibiotics. The high concentration of antibiotics will effectively treat even relatively resistant Chlamydia trachomatis strain. We believe, a large number of male pelvic infections is caused by or aggravated by Chlamydia infection. The sonographic guidance allows injecting the antibiotics precisely into the most affected areas. The side effects of the antibiotics are not a concern. The procedure extremely well tolerated.
Unilateral or bilateral injections for the prostate?
As the attached sonogram picture will show (Figure 2), in a structurally intact prostate, unilateral injection promptly results in bilateral filling of both lobes of the prostate. If scarring is obvious in both lobes targeted delivery of antibiotics is recommended. Transrectal delivery of antibiotics is exceptionally suitable for this method.Factors influencing the chances for a complete cure of chronic pelvic infections in the male:
- Duration of the disease.
- Number of different antibiotic regimens administered and the total length of therapy. The prevalence of multi-drug resistant bacteria is a significant and growing concern.
- Sonographic appearance of the prostate, seminal vesicles, epididymis and testes. The extent of scarring is inversely related to positive therapeutic outcome.
Potential complications
Local discomfort during the procedure. (By far less then the discomfort associated with tranperineal injections.) Easily managed by non steroidal pain medications. Mild hematuria and hemospermia that may last for three to four weeks. Mild transient bleeding from hemorrhoids.Follow up
One month following the therapy the symptom evaluation, cultures, and sonography examinations are repeated.Change in symptom index:
All of our patients who reported for therapy within days of acquiring the infection showed complete reversal of symptom scores within days. The majority with chronic symptoms still experienced 60 to 80 % long-term improvements and complete recovery is not a rarity. Often, residual symptoms further improved by the three to six months post therapy evaluation.
Change in post therapy bacteria count: There is consistently a precipitous drop in the bacteria colony count in the post therapy semen samples.
Booster injections
We recommend individually planned booster injections at three, six and nine months following the initial therapy. Symptom flare ups can prompt administration of booster injections any time much sooner.The question of EDTA
Adding EDTA to the injected mixture to dissolving calcium salt is based on a chemical fact that EDTA, being a chelating agent, will dissolve calcium salts.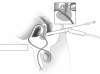
Figure 1. Transrectal injection of antibiotic cocktail into the prostate. Note the proximity of prostate to the rectal wall and the precise targeting of injection. (Click on to enlarge)

Figure 2. Unilateral injection of Erythromycin succinate emulsion into the prostate. Prompt filling of bilateral prostatic ducts are visualized in structurally intact prostate. This finding supports the notion that unilaterally given one injection in structurally intact prostate is probably sufficient. (Click on to enlarge)

Figure 3. Five Years Follow Up on the First 66 Patients Treated with Trans Rectal Injections. (Click on to enlarge)

Figure 4. % Improvement After Trans Rectal Antibiotic Injections . (Click on to enlarge)
Figure 5. Video showing a typical injection procedure. (Click on to play)
For more information on etiologies of chronic prostatitis click here. Because standard medical protocol often fails to address chronic prostatitis, many alternative therapies have been developed. These have varying degrees of credibility and efficacy. More information provided below —
Saw Palmetto
Allopurinol
Quercetin and Other Bioflavonoids
Elmiron
Prostate Massage and Drainage
Injection Therapy
Etiology of Acute Prostatitis
Etiology of Chronic Prostatitis
Non-bacterial Prostatitis
Chlamydial Prostatitis



